- Sections :
- Crime & Public Safety
- Restaurants & Food
- Sports
- More
COVID-19 Vaccine Questions Answered by Houston Methodist The Woodlands Hospital Employees Who Received the Vaccine Last Week
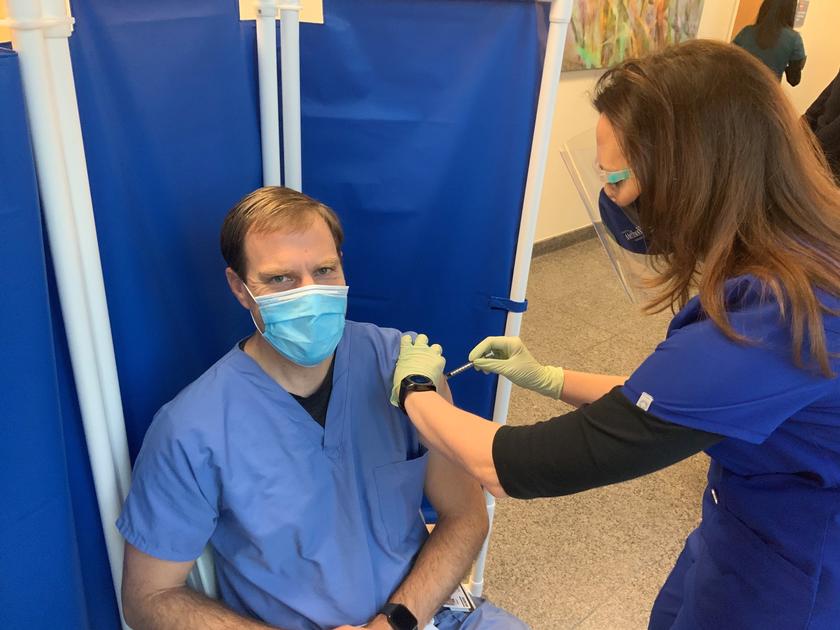
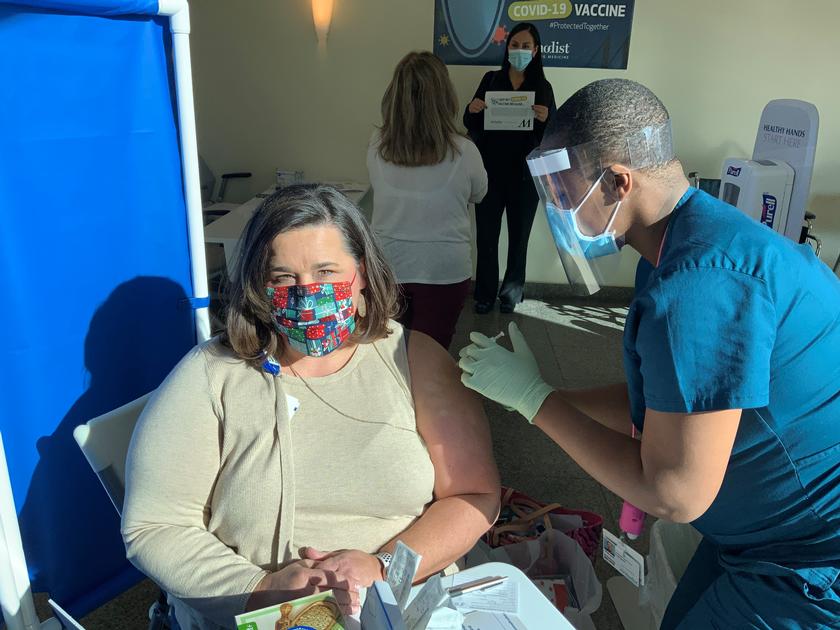
THE WOODLANDS, TX -- Frontline employees at Houston Methodist The Woodlands Hospital received the recently approved COVID-19 vaccine by Pfizer and BioNTech, December 16. The vaccine is a lipid nanoparticle, or, in layman's terms, a small particle of fat. Residing inside of that nanoparticle is messenger RNA (ribonucleic acid). Cells use messenger RNA (mRNA) to make proteins; when injected into a person’s body, the mRNA merges with a cell and tells it to create a particular protein. In this case, it creates the spike protein on the surface of COVID, and since this is a foreign protein, the body subsequently produces antibodies that result in an immense immune response.
“The reason it's such a brilliant and simple solution is it uses your body's own existing internal infrastructure to make immunity without getting infected or sick,” said Dr. Jason Knight, Chief Medical Officer at Houston Methodist The Woodlands. “It's not a dead virus. It's not a live virus. It's not an attenuated virus. It's not a chimpanzee virus. It's not DNA, it doesn't alter your genetics … and the cool thing is, after it's used up, the messenger RNA goes away. So it's not even permanently in your body.”
The following is a Q&A with Dr. Jason Knight, Chief Medical Officer at Houston Methodist The Woodlands:
Should I get the vaccine if I’ve already had COVID-19?
'What we have found is that when people get sick with COVID-19, they get a certain level of immunity, and then after about three months, that immunity can start to wane … Some people are still immune for six, or eight months … so we are recommending that even people that got COVID, in the beginning of this pandemic, February, March, April, they should get their vaccine. And if you've had it more recently, like say, November and December, we recommend waiting three months and then getting the vaccine.'
Is the vaccine safe?
'The vaccine is incredibly safe. It is essentially 100% effective in preventing people from being admitted to the hospital with COVID-19 … no one that got the vaccine died or ended up in the ICU or on a ventilator.'
What are the most common side effects?
'The side effect profile is really good. About 2% of people will develop a low-grade fever or a fever. Two out of 102% of people will get a headache; about 4% of people will get some fatigue, and 2 to 4% of people will get some muscle aches or some body aches or a sore shoulder near the injection site.'
What about those who have experienced an allergic reaction because of the vaccine?
'These have all been people that have had multiple severe allergic reactions in the past. I think if you're someone that has had multiple severe allergic reactions in the past, you should check with your allergist or your doctor before you get the vaccine. But I did have an ER nurse this morning that I've known for quite some time who falls in that category. She’s had over 20 admissions to the hospital for severe allergic reactions in the past, and we just pre treated her with Benadryl and Tylenol and she did great.'
There has been speculation surrounding the vaccine and infertility - is there any truth to this claim?
'That's totally ridiculous because it has nothing to do with sperm production or how the uterus works, or getting pregnant, or anything like that.'
What about complications with pregnancy?
'There's a lot of discussion about pregnancy. We don't have a lot of data in pregnancy, which is why the UK didn't approve it. It's not that it's dangerous. It's not that it's bad. It's not that pregnant women had a problem with it. It's just that we don't have enough data yet.'
Once I get the vaccine, will I still have to follow CDC guidelines currently in place?
'Even if you get the vaccine, you're still going to have to wear a mask, you're still going to have to wash your hands, you're still going to have to social distance for a little while, because, though we know that the vaccine is very effective in preventing severe disease and hospitalization and death and ventilators, we're not sure if people can still get infected with COVID and potentially spread it for a few days before their immune system clears it - kind of like an asymptomatic spreader.'
Could I still contract COVID-19 after receiving the vaccine?
'We don't know if people are still going to be able to be infected or not, but it's definitely true that it's not going to be as severe.'
How is the vaccine administered?
'It is a two-vaccine regimen. So, you get one initial injection, and then 19 to 23 days later, you get the second injection. You get about 50% immunity 10 to 14 days after the first injection. And then you get up to 100% immunity around 10 to 14 days after the second injection. Both are injected into the patient’s shoulder.'
Within the general public, who will receive the vaccine first?
'If you're 65 and have a lot of medical problems, and you're generally pretty sick, you're going to be in Tier One, and you're going to get vaccinated sooner. If you're a 20-year-old athlete who's super healthy, you're going to be at the very bottom. And basically, everybody else is kind of in between. So the older you are and the sicker you are, the higher priority you're going to be in getting the vaccine first.'
Why should I get vaccinated?
'The number one reason to get vaccinated, I think, is that we all have a personal responsibility to not only take care of our own health, but to take care of the health of our friends and family, to take care of the health of our colleagues, to take care of the health of all of our patients, especially in the hospitals, and to take care of the health of the community at large … I've tried for 11 months not to die from COVID, and not to bring COVID to my wife and five kids and my elderly parents, and it was just an amazing experience to get the vaccine. So I do hope people choose to get vaccinated.'
Dana Hamons, RN at Houston Methodist The Woodlands, also received the vaccine. She said that it was quick, easy, and painless. “You know, sometimes the flu vaccine, it burns or you feel something. I didn't have any kind of discomfort [with the COVID vaccine] when she gave me the injection, and it was over before I could blink it off,” she said.
“The people that have had lesser amounts of COVID disease, that have been able to be treated at home, I don't see those. I see the people that are so incredibly, profoundly sick, the people that are struggling to breathe, the people that are bereft because their families can't be at their bedside with them. And they're scared … We have encountered that type of COVID,” Hamons said.
'I'm a nurse of 27 years, let me assure you, I read through all of the information, but when I had to weigh what it meant for me to take the vaccine versus taking the chance of having COVID from the angle and the vantage point that I've had at the bedside ... taking the vaccine was the lesser risk,” she said.
“We want to strongly encourage that we know that wearing a mask makes a difference. And that washing your hands and wearing your mask over your nose and your mouth are the most important tools until others can receive the vaccine … Is this the end of COVID? No, but is it the beginning of the end? I think it’s a new chapter. It's the first ray of hope that we have had,” she said.