Now Is The Time Re-Shop Your Medicare Supplement Insurance

NOW IS THE TIME TO RE-SHOP YOUR MEDICARE SUPPLEMENT INSURANCE
Posted on June 7, 2023
JUNE 7 2023
By D. Kenton Henry – editor, broker
Everyone with Medicare Supplement knows the value and convenience it provides in allowing the policyholder to seek medical attention from any medical provider that sees Medicare patients. All hospitals see Medicare patients, so, heaven forbid, should we get cancer and want to go to MD Anderson Hospital in Houston—we may go directly there. And, depending on which Medicare Supplement plan we elect, we can be out of virtually nothing for our medical care.
The only real disadvantage to a Medicare Supplement plan is the premium. And it's not the first-year premium upon entering Medicare at age 65, but rather the premium in the ensuing years. This occurs because, as we age, each year, on our policy anniversary, the premium is usually increased to account for the additional risk an insurance company assumes to cover us as we age. The older we are, the more likely we are to generate medical insurance claims, and larger ones at that. Hence, the older we get, the more burdensome our premiums will become.
The only solution to that (while remaining insured)—other than to switch to a Medicare Advantage plan—is to re-shop our supplement plan. Typically, it does not behoove us to do this every year. Assuming our insurance company is ethical and competitive, the savings involved in moving to a more competitive plan won't be large enough to warrant the effort. But by the time we have experienced a second or third annual increase—it will be. In only a few states, is a Medicare Supplement policyholder allowed the right to move to a lower-cost plan and be guaranteed approval. This transition will be accomplished during that state's Open Enrollment Period. Texas has no Open Enrollment Period for Medicare Supplements. In Texas, Open Enrollment only applies to Medicare Advantage and Part D Drug Plans. In Texas, a Medicare recipient can apply for a new Medicare Supplement policy 365 days per year. Still, they must qualify based on their current health and health history. If their health is good, or their medical conditions are well controlled, they may be approved for the new and lower-cost plan. And this can be accomplished while maintaining equal benefits or even upgrading to superior benefits, if available.
If you are wondering if lower-cost Medicare coverage is available and considering applying for such—now is the time to do so. Brokers and agents, like myself, are currently in our slow period. This is because the government (Medicare) dictates when Medicare recipients may apply for a Medicare Advantage or Part D Drug Plan. That is each year between October 15 and December 7—the Open Enrollment Period for those products. Plans applied for during that period are guaranteed approval with a January 1 effective date. Brokers and agents who specialize in Medicare-related insurance products, like myself, begin studying and testing for national tests, which must be passed each fall in order to represent these plans in the coming calendar year, along with certifying (testing) with each insurance company whose product we want to represent. So from September, when most of us study and test, to the end of December, we are inundated with identifying our client's best plan options for the coming year and enrolling them in that product. Even with the best of staff, our market feels as though we are surrounded by "sharks in a feeding frenzy." Especially if we also assist Under Age 65 clients in obtaining Individual and Family health insurance with an overlapping Open Enrollment Period!
So—if you are at all considering obtaining a lower-cost Medicare Supplement plan—now—and the next three months—is the time to do so. I can scan the market to identify equal or superior benefits at meaningful premium savings. Sometimes a very meaningful 30% or more! Once I have done that, I will make the application process go as quickly and smoothly as possible. I charge no fee for my service, and you will be charged no more for the insurance plan than if you acquire it directly from the insurance company itself. You will not cancel your current coverage until we know you have been approved for all pre-existing conditions.
Please email or give me a call. I have been in the industry for 37 years and am not going anywhere. I enjoy what I do, and that is helping others find their best medical coverage at the lowest possible cost.
*(Please see feature article 1 below on prescription drug shortages and feature article 2 on Medicare Advantage Claim Denials.)
D. Kenton Henry
Office: 281-367-6565 Text my cell 24/7: 713-907-7984 Email: Allplanhealthinsurance.com@gmail.com
*(comment box)
Https://HealthandMedicareInsurance.com Https://TheWoodlandsTXHealthInsurance.com Https://Allplanhealthinsurance.com
**********************************************************************
FEATURE ARTICLE 1
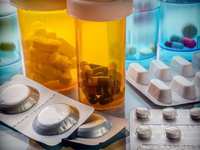
Drug price caps in Inflation Reduction Act exacerbating shortages, Gottlieb says . . .
THE HILL
BY JULIA SHAPERO - 05/21/23 4:58 PM ET
Former Food and Drug Administration (FDA) Commissioner Scott Gottlieb
Former Food and Drug Administration (FDA) Commissioner Scott Gottlieb said on Sunday that drug price caps in the Inflation Reduction Act are exacerbating drug shortages.
"The features under the Inflation Reduction Act will exacerbate this problem, because it'll prevent these generic manufacturers from being able to take price increases," Gottlieb, who now serves on the board of Pfizer, told CBS' "Face the Nation."
"For example, if they enter a market for the first time, or they spend a lot of money upgrading a facility to be compliant with state-of-the-art regulations, they're not gonna be able to take a price increase to recoup some of those costs," he added. "So, it's going to come out of their own pocket."
Gottlieb said that sterile injectable drugs are particularly susceptible to shortages, suggesting that they should be carved out of the Inflation Reduction Act.
"The reimbursement for these drugs under government programs has been driven down very low, something above the marginal cost of manufacturing the drugs, and that's fine when it comes to a pill form drug where there's not a lot that can go wrong."
"But when it comes to an injectable drug, you need to leave a margin in so people can reinvest in manufacturing facilities, make sure they're high quality," he added. "They haven't done that, and things go wrong, and it results in shortages."
A March report from the Senate Committee on Homeland Security and Governmental Affairs found that there were more than 295 active drug shortages at the end of 2022, marking a five-year high.
**********************************************************************
FEATURE ARTICLE 2
SENATORS PRESS MEDICARE ADVANTAGE INSURERS OVER CLAIMS DENIALS
FIERCE HEALTHCARE MAY 19, 2023
By Paige Minemyer
There were no insurers represented on the hearing panel, and the senators instead heard from multiple policy experts, the Office of Inspector General and the widow of a patient who was harmed by care denials and delays. (Getty Images/designer491)
Pharmacy benefit managers weren't the only ones on the hot seat in Congress this week.
The Senate's Permanent Subcommittee on Investigations put Medicare Advantage (MA) plans on notice Wednesday, demanding answers for claims denials. Chairman Richard Blumenthal, D-Connecticut, said in an opening statement during the hearing that the committee sent letters to the three largest MA plans—UnitedHealthcare, Humana and Aetna—seeking documentation on how they make decisions around claims denials.
Blumenthal said these coverage denials have become commonplace for many MA enrollees.
"These denials have become so routine that some patients can predict the day on which they will come," he said.
He added that "there is growing evidence" pointing to MA plans using artificial intelligence and data algorithms in making denials, rather than relying on feedback from physicians or other clinical experts. A recent investigation from Stat found that these tools are taking on an increasing role in coverage decisions, though there is limited oversight and transparency
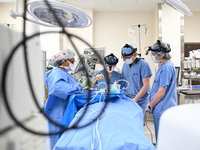
Blumenthal said the Department of Health and Human Services Office of Inspector General (OIG) has also identified a "large number of cases" where MA insurers refused to authorize services that met coverage requirements under Medicare. For example, a cancer patient seeking a routine scan to determine whether the disease had spread was held up by their insurer for a month, and another payer refused to cover a walker for a patient as they had already received a cane.
"In each of these cases, the insurer's decision overlooked the treating physician's assessment of what their patient needed," Blumenthal said.
There were no insurers represented on the hearing panel, and the senators instead heard from multiple policy experts, OIG and the widow of a patient who was harmed by care denials and delays. Megan Tinker, chief of staff at OIG, said in her submitted statement that in 2018, MA plans denied 1.5 million prior authorization requests, about 5% of the total. In addition, they rejected 56.2 million payment requests, or 9.5%.
Tinker said that between 2014 and 2016, MA plans overturned their own coverage denials 75% of the time when a member or provider appealed the decision. OIG also found that 13% of coverage denials were for services that met Medicare's coverage rules.
Tinker noted in her opening remarks that the program has grown rapidly over the past several years, and enrollment in MA now accounts for more than 50% of total Medicare enrollment.
"Fast growth has increased vulnerabilities and the need for robust program integrity measures," she said. "OIG work has demonstrated that the risk of waste, fraud and abuse in managed care are significant."
Jean Fuglesten Biniek, Ph.D., associate director of the Program on Medicare Policy at KFF, noted in her submitted remarks that the way payments work in MA may create financial incentives for insurers to deny care. It costs MA plans 83% of what it costs traditional Medicare to cover key services, while they are paid 106% of what the Centers for Medicare & Medicaid Services pays in fee-for-service Medicare, according to data from the Medicare Payment and Advisory Commission.
This means plans retain $2,300 above the cost of paying for a member's care, she said.
She added that there are also significant gaps in the data around prior authorization in MA; for example, there is no information about what services are denied or whether there are certain beneficiaries who are denied care more often. There is also a dearth of detail on how long it takes MA plans to respond to these requests.
"As a result, policymakers don't have the information they need to conduct oversight," she said.